According to the World Health Organization (WHO), approximately 332 million people suffer from depression globally, which is about 4% of the population. It’s 1.5 times more prevalent in women than men. For many people, standard treatments, such as antidepressant medication, lifestyle changes and psychotherapy can bring relief, especially over longer periods of time. However, some individuals don’t respond the same, nor experience any meaningful results.
Treatment resistant depression – what is it? Definition & clarifications

Treatment resistant depression or TRD is a type of major depressive disorder that doesn’t show signs of significant improvement after at least two different antidepressant medications have been administered over a sufficiently long period of time. For example, if a person experiences 25% or less of a reduction in symptom severity over 6-8 weeks of conventional treatment, or, in other cases, if the symptoms seem to improve temporarily but return afterwards. Around 30% of people diagnosed with major depressive disorder experience TRD.
Most providers prescribe SSRIs (selective serotonin reuptake inhibitors), SNRIs (serotonin and norepinephrine reuptake inhibitors), bupropion and mirtazapine as first-line medications for depression.
The exact cause of TRD is not known, but contributing factors may be genetics, brain chemistry and stress, which affects the hypothalamic-pituitary-adrenal (HPA) axis. The HPA axis is responsible for our body’s adaptation to stress, and chronic stress especially may worsen depression and make it more difficult to treat. Other risk factors include autoimmune, thyroid, heart and cerebrovascular diseases.
Treatment resistant depression symptoms
Treatment resistant depression manifests very similarly to other types of depression. The core difference is that it doesn’t improve, even when applying a mix of different therapies and antidepressant medical treatments. Additionally, a longer duration of depressive episodes can be seen, sometimes accompanied by other symptoms such as insomnia.
Affected individuals may experience:
- Persistent low mood and feelings of sadness, anxiety or hopelessness
- Loss of interest or pleasure in hobbies and activities
- Fatigue and changes in sleep patterns (insomnia or hypersomnia)
- Feelings of worthlessness, irritability and restlessness
- Difficulty concentrating or feeling slowed down mentally
- Suicidal ideation
TMS as one of the most promising treatment resistant depression treatments
Living with severe depression that doesn’t respond well to conventional treatment plans can be a very hard and isolating experience. That is why many clinicians often look towards advanced methods, including TMS (Transcranial Magnetic Stimulation).
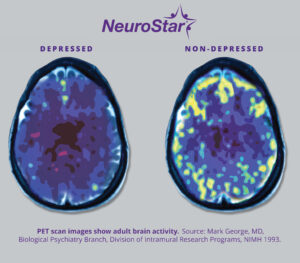
TMS is a non-invasive, FDA-approved therapy that uses magnetic pulses to stimulate specific areas of the brain involved in mood regulation, usually the left dorsolateral prefrontal cortex (DLPFC). This process is meant to stimulate the areas that are underactive in individuals with depression.
At Neurovana, we specialize in providing TMS treatments for multiple conditions, including depression, PTSD, OCD and anxiety. According to a TMS study conducted by Harvard Health, 50%-60% of those who have tried and haven’t experienced relief from antidepressive medications have had a positive clinical response from TMS therapy, and a third of them benefitted from full remission.
As opposed to medication which has an effect on the entire body, TMS specifically targets the neural circuits associated with depression, it doesn’t require anesthesia, nor does it cause systemic side effects.
When can I expect results from TMS if I have treatment-resistant depression?
TMS aims to rewire the connection between the brain regions responsible for mood regulation, attention and behavior. It’s a targeted procedure, with one session typically lasting 18-20 minutes, and treatment is administered 5 days a week, for 6-7 weeks, so around 36 sessions total. Most patients already start noticing improvements within 2-4 weeks, though results may vary for each individual.
TMS is non-invasive, meaning that no injections, incisions or anesthesia are involved. You are fully awake, alert and in control, and after the session is over, you can return to your activities, which makes TMS a very attractive treatment option.
Furthermore, TMS is a flexible treatment plan that can also be used in conjunction with other therapies, such as counselling.
TMS promotes neuroplasticity, or encourages the brain to form new neural pathways, which can help break patterns of depressive thinking and improve emotional regulation. It also doesn’t affect hormones, sleep patterns or cognition. The side effects of a TMS session are minimal, in most cases a headache or mild scalp discomfort.
Who is a candidate for TMS? Find out if it’s the right option for you
If you’ve battled depression for a long time and have tried multiple medications with no success, then you could definitely be a candidate for TMS. Generally, TMS is prescribed to adults aged 18 and over and adolescents aged 15 and over. It can also be a great fit for those who can’t tolerate the side effects of regular antidepressant medication. If you have PTSD or OCD, you might also benefit from being evaluated for TMS, as you could receive relief for multiple mental health conditions.
Book a consultation with us at Neurovana to explore why TMS could be a game-changer for you and start reclaiming your life and happiness.